We focused on a peptide therapy in cytoprotection, using a small, orally active, anti-ulcer peptide (6, 9-11), stable in human gastric juice (12) with significant cytoprotective activity (6, 10, 11) - stable gastric pentadecapeptide BPC 157 (MW 1419), with very safe profile (LD1 could be not achieved, no side effects in clinical trials (13, 14), effective in trials for inflammatory bowel disease therapy (13, 14) and wound healing (15-18). Previously, BPC 157 was found to particularly protect endothelium (10), angiogenesis (16) and modulate NO-system function (i.e., L-NAME-induced hypertension was prevented and reversed by BPC 157 application) (11, 19). Importantly, pentadecapeptide BPC 157 was more active than recombinant human platelet-derived growth factor (PDGF-BB), stimulating both expression of early growth response 1 (egr-1) gene and its repressor nerve growth factor 1-A binding protein-2 (NAB2) (18). Also, pentadecapeptide BPC 157 was found to improve healing of ileo-ileal, colo-colonic, ileo-jejunal (20, 21) anastomosis and gastrocutaneous and colocutaneous fistulas (20, 22). Very recently pentadecapeptide BPC 157 was found to improve healing of transected sciatic nerve in rats, applied intraperitoneally/intragastrically/locally, at the site of anastomosis, or after non-anastomozed nerve tubing directly into the tube (23).
Animals
Male Albino Wistar (350-400 g) rats, were used in all of the experiments (10 rats at least per each experimental group and interval randomly assigned) approved by the Local Ethic Committee and assessed by observers unaware of the given treatment. Abdominal aorta anastomosis creation. Procedure includes deeply anesthetized rats, prone position, cleaned operative field, median incision, exposing the retroperitoneum, identifying the structures, preparation of the aorta, placing the clamps, horizontal cut between renal arteries and bifurcation (common illiac arteries) and termino-terminal anastomosis creation (8/0 Prolene sutures) (i.e., with 20 minutes of complete ischemia) (Fig. 1).
 |
Fig. 1. Procedure of abdominal aorta anastomosis. A. Preparation of the aorta, placing the vascular clamps. B. Horizontal cut between renal arteries and bifurcation (common illiac arteries). C. Starting the anastomosis, first sutture. D. Releasing the clamps, checking the distal pulse. Period A-D 20 minutes. |
Drugs
Medication, without carrier or peptidase inhibitor, includes pentadecapeptide BPC 157 (a partial sequence of human gastric juice protein BPC, freely soluble in water at pH 7.0 and in saline; peptide with 99% (HPLC) purity (1-des-Gly peptide as impurity, manufactured by Diagen, Ljubljana, Slovenia, GEPPPGKPADDAGLV, M.W. 1419 prepared as described before (9).
Experimental procedure includes an (i) application to attenuate or prevent thrombus formation as well as (ii) an application in the conditions of the already established thrombus (24 h post-surgery). BPC 157 (10 µg/kg) was given (i) as a bath immediately after anastomosis creation, or (ii) intraperitoneally at the 24 h after surgery. Control received an equivolume of saline (5 ml/kg).
Functional evaluation
Function disability was assessed as described before (16, 17). Briefly, Kokas extensor postural thrust (EPT) i.e., modified motor function index (MFI) assessed by an experienced, but naive, co-tester, as the weight on a digital weighing scale (precision 0.001 g) borne by the hind limb at the moment when the rat was held upright, with the hind limb extended and placed upon a scale, begins to bear weight on the scale, as follows: EPT = (NEPTEEPT)/NEPT (NEPT and EEPT represent EPT value before surgery (normal) and after surgery (experimental), respectively).
Walking ability was scored (1-3) using a simple modification of the previous assessment as follows: 1 - normal walk, optimal speed, no tottering; 2 - slow, but still normal walking, no tottering; 3 - tottering walk with either spontaneous or induced vocalization; 4 - the animals unable to walk, with either spontaneous or induced vocalization.
The first assessment was before surgery. The second assessment was at the 24 h post-surgery before sacrifice or therapy administration. Those rats that received medication at the 24 h post-surgery were assessed also at the 1 min and then at the 3 min thereafter, before sacrifice.
Microscopical assessment
Part of the interest of the aorta (length of cca. 2 cm) was placed in buffered formalin (pH 7.4) immediately after removal from the animal sacrificed at 24 h after surgery or alternatively, in those rats that received medication at 24 h after surgery at 3 minutes after medication. Sutured segments were cut, dehydrated, and embedded in paraffin wax so that the whole length of this segment could be sectioned. Aorta samples were cut serially at the thickness of 5 µm, stained with hematoxylin and eosin, and analyzed in a blinded fashion. Three segments of each sample with the largest lumen obstruction were selected and using a video camera (Sony TK1270) put into ISSA database. These images were used for morphometrical assessment of the lumen occlusion using special program ISSA (VAMSTEC, Zagreb, Croatia). In each segment total area of the lumen and total area of the thrombus were measured, with final result expressed as percentage of lumen occupied with thrombus.
Statistical analysis
Statistical analysis was performed using program GraphPad Prism 5.0. for Windows. Categorical data were analyzed using Kruskal-Wallis and post hoc Mann-Whitney U test. Values are expressed as min/med/max. Test results with P<0.05 were considered statistically significant.
Statistical analysis of the quantified data was performed by analysis of variance (ANOVA). Post hoc comparisons were appraised using the conservative Bonferroni/Dunn test. Data are presented as mean±standard deviation (SD). Values of P£0.05 were considered statistically significant.
Assessment at 24 h after surgery
The end to end aortal anastomosis procedure invariably lead to significant thrombus formation and aortal lumen occlusion and prominent edema in vessel wall, unless BPC 157 was applied immediately after anastomosis creation (Fig. 2, Table 1). BPC 157 demonstrated significantly lower percentage of aortal lumen occlusion with thrombus and less edema in vessel wall. Also, the walking ability was markedly impaired, accompanied with painful vocalization, either screaming spontaneous or at very light touch, and very weak muscle strength, unless BPC 157 was applied. Along with less thrombus formation and less aortal lumen occlusion pentadecapeptide BPC 157 animals exhibited preserved walking and muscle strength (close to normal) (Fig. 2, Table 1).
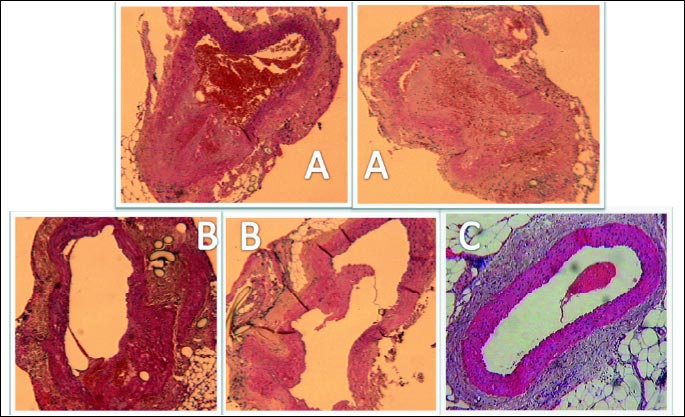 |
| Fig. 2. Transversal sections of aorta (HE, x2). A, B. Assessment at 24 h after after anastomosis creation. Significant thrombus formation and aortal lumen occlusion (control rats) (A), unless BPC 157 (10 µg/kg bath) (B) had been applied immediately after anastomosis creation. (C). Medication at 24 h after surgery and subsequent assessment. In animals treated with BPC 157 (10 µg/kg i.p.) 24 hours after surgery, at the time of sacrifice (3 minutes after treatment) there was no obvious aortal occlusion, and only erythrocytes were present in the lumen (C). |
Medication at 24 h after surgery and subsequent assessment
As indicated, at 24 h aortal anastomosis rats were presented with significant thrombus formation and aortal lumen occlusion, markedly impaired walking ability, painful vocalization, and very weak muscle strength.
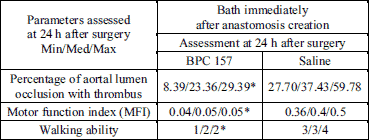
| Table 1. Assessment
at 24 h after surgery. BPC 157 (10 µg/kg) was given as a bath immediately
after anastomosis creation. Control received an equivolume of saline (5
ml/kg). *P |
 |
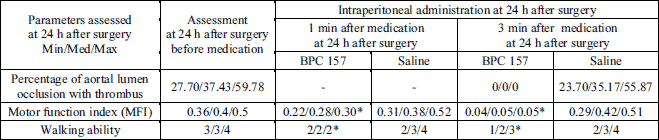
| Table 2. Medication at 24 h after surgery and subsequent assessment. BPC 157 (10 µg/kg) was given intraperitoneally at the 24 h after surgery. Control received an equivolume of saline (5 ml/kg). Assessment at 1 and 3 min after medication. |
 |
In strong contrast, in animals treated with BPC 157 24 hours after surgery, at the time of sacrifice (3 minutes after treatment) there was no obvious aortal occlusion, and only erythrocytes were present in the lumen. Intriguingly, BPC 157 administration rapidly induced walking ability improvement, and an increase of muscle strength; the moment when the muscle strength reached the values of the normal rats was used to determine the point of the thrombus assessment and the animals were sacrificed at 3 min after medication (Fig. 2, Table 2).
This is the first study that presumes the problem of aorta abdominalis anastomosis to be additionally elucidated within the concept of stomach cytoprotection and cytoprotection/endothelium protection relation, the endothelium protection equally relevant for both cytoprotection and abdominal anastomosis outcome.
Consequently, an essential cytoprotective activity and endothelium protection of BPC 157 (6, 9-11) that may be useful also in major vessels injuries may be likely. In support of this notation, we substantiated an evident effect in the worst conditions that may be presented throughout abdominal aorta anastomosis, at time of creation, immediately after surgery, as well as at the time of established thrombus and markedly injured limbs function. Namely, BPC 157 may decrease formation of cloth after aortic termino-terminal anastomosis in rats when given as a bath immediately after aortic anastomosis creation. Also, there was no cloth found in rats at the anastomosis site when BPC 157 given at the point of 24h post-surgery, in the conditions of the already established thrombus at the site of anastomosis. Thus, we have an immediate benefit of BPC 157 when given as a bath immediately after anastomosis creation that was however assessed after 24 hours. Likewise, we showed a comparable effect of an intraperitoneal injection that was postponed at that point of 24 h post-surgery. These both imply both rapid and sustained effect.
Finally, BPC 157 beneficial effect is closely supported with the improved limbs function (of note, the function recovery in muscle injuries may be the earliest healing hallmark (17)). Accordingly with aortic surgery limbs ischemia in patients (i.e., that may be associated with a high morbidity and mortality (3)) abdominal aorta anastomosis significantly impaired rats limbs function, i.e., only one half of initial muscle strength remained (surprisingly, previously little investigated in rats (2). At 24 h post-surgery, BPC 157 rats with less obstruction exhibited ameliorated limb muscle strength similar to those values before the surgical procedure. Interestingly, given at the that postponed point of 24 h post-surgery, BPC 157 rats had no cloth at the anastomosis site at the time when the function of lower limbs was completely rescued.
Previously, as far the blood vessels integrity may be considered, already since the earliest post-injury intervals, BPC 157 was found to be an effective therapy. BPC 157 may inhibit and reduce posttraumatic hematoma formation in rats subjected to crush muscle injury while rapidly improve function of the injured leg in rats with both muscle transection and crushed muscle (16, 17). BPC 157 usefully improved deep burns healing, and therefore, dermal vascular changes following thermal trauma resulting in fibrin deposition and vascular occlusion at the site directly destroyed by thermal energy and changes in dermal haemodynamics and blood vessel morphology in the areas of dermis surrounding the burn area (15). Also, while improving intestinal anastomosis healing BPC 157 exhibited formation adhesions attenuated, blood vessels fulfilled, mild passage obstruction only temporary (otherwise, along with intestinal passage obstruction, filling of vessels with blood tends to deteriorate, and vessels become empty) (24). This may be important presenting that intestinal anastomosis healing requires improved abdominal aorta blood flow (25). Similar to that, when BPC 157 was given intragastrically, the fulfilled blood vessels were also presented throughout maximal stomach distention (26), and gastric mucosal blood flow was increased at the ulcer margin (27). Intriguingly, BPC 157 was also found to reduce bleeding time while it has no effect on clothing parameters in vitro (9). Also, BPC 157, like other cytoprotective agents, markedly reduced the presentation of bleeding ulcer after restraint stress, NSAIAs or alcohol (6, 10, 11). Unfortunately, our study did not investigate the effects commonly thought (for review see, (25)) to cause endothelial damage such as decrease in the relaxing effect of NO/EDRF (28), ADP, thrombin, Ca2+-ionophore A-23187 on endothelium; increase in platelet aggregation and turnover as well as the sensitivity of platelets to aggregating substances due to the modification of effects of PGI2 and TXA2; increase in the release of endothelium-derived vasoconstrictor substances such as serotonin and TXA2 through the cyclooxygenase pathway. Thereby, because of particularly protecting endothelium, angiogenesis and modulating NO-system function (i.e., BPC 157 may induce a NO release resistant to L-NAME-application) (11, 19), maintaining ATP content in stomach mucosa (29), reducing inflammatory mediators and Ca2+-ionophore A-23187 effects (30, 31), BPC 157 effects (both prevention and reversal of thrombus in abdominal aorta after surgery) may be interesting for further studies. For instance, pentadecapeptide BPC 157, by stimulating both expression of egr-1 and its repressor NAB2 (18), may represent a controlling mechanism that may be responsible for regulation of egr-1. This may be important probably not only in theory presenting that egr-1 is associated with intraluminal thrombus formation in human abdominal aortic aneurysm (32).
Conflict of interests: None declared.
- Haraguchi T, Okada K, Tabata Y, Maniwa Y, Hayashi Y, Okita Y. Controlled release of basic fibroblast growth factor from gelatin hydrogel sheet improves structural and physiological properties of vein graft in rat. Arterioscler Thromb Vasc Biol 2007; 27: 548-555.
- Sako H, Hadama T, Miyamoto S, et al. Effect of prostaglandin E1 on ischemia-reperfusion injury during abdominal aortic aneurysm surgery. Surg Today 2006; 36: 140-146.
- Kuhan G, Raptis S. Trash foot following operations involving the abdominal aorta. Aust NZJ Surg 1997; 67: 21-24.
- Robert A. Cytoprotection by prostaglandins. Gastroenterology 1979; 77: 761-767.
- Szabo S, Trier JS, Brown A, Schnoor J. Early vascular injury and increased vascular permeability in gastric mucosal injury caused by ethanol in the rat. Gastroenterology 1985; 88: 228-236.
- Sikiric P, Seiwerth S, Deskovic S, et al. New model of cytoprotection/adaptive cytoprotection in rats: endogenous small irritants, antiulcer agents and indomethacin. Eur J Pharmacol 1999; 364: 23-31.
- Kwiecien S, Pawlik MW, Brzozowski T, et al. Nitric oxide (NO)-releasing aspirin and (NO) donors in protection of gastric mucosa against stress. J Physiol Pharmacol 2008; 59(Suppl 2): 103-115.
- Brzozowski T, Konturek PC, Pajdo R, et al. Physiological mediators in nonsteroidal anti-inflammatory drugs (NSAIDs)-induced impairment of gastric mucosal defense and adaptation. Focus on nitric oxide and lipoxins. J Physiol Pharmacol 2008; 59(Suppl 2): 89-102.
- Sikiric P, Petek M, Rucman R, et al. A new gastric juice peptide, BPC. An overview of the stomach-stress-organoprotection hypothesis and beneficial effects of BPC. J Physiol (Paris) 1993; 87: 313-327.
- Sikiric P, Siwerth S, Grabarevic Z, et al. The beneficial effect of BPC 157, a 15 amino acid peptide BPC fragment, on gastric and duodenal lesion induced by restraint stress, cysteamine and 96% ethanol in rats. A comparative study with H2 receptor antagonists, dopamine promoters and gut peptides. Life Sci 1994; 54: 63-68.
- Sikiric P, Seiwerth, S, Grabarevic Z, et al. The influence of a novel pentadecapeptide, BPC 157, on N(G)-nitro-L-arginine methylester and L-arginine effects on stomach mucosa integrity and blood pressure. Eur J Pharmacol 1997; 332: 23-33.
- Veljaca M, Chan K, Guglietta A. Digestion of h-EGF, h-TGF alpha and BPC 157 in human gastric juice. Gastroenterology 1995; 108: 761.
- Veljaca M, Pavic-Sladoljev D, Mildner B, et al. Safety, tolerability and pharmacokinetics of PL 14736, a novel agent for treatment of ulcerative colitis, in healthy male volunteers. Gut 2003; 51: A309.
- Ruenzi M, Stolte M, Veljaca M, Oreskovic K, Peterson J. Ulcerative Colitis Study Group. A multicenter, randomized, double blind, placebo-controlled phase II study of PL 14736 enema in the treatment of mild-to-moderate ulcerative colitis. Gastroenterology 2005; 128: A584.
- Sikiric P, Seiwerth S, Mise S, et al. Corticosteroid-impairment of healing and gastric pentadecapeptide BPC-157 creams in burned mice. Burns 2003; 29: 323-334.
- Novinscak T, Brcic L, Staresinic M, et al. Gastric pentadecapeptide BPC 157 as an effective therapy for muscle crush injury in the rat. Surg Today 2008; 38: 716-725.
- Staresinic M, Petrovic I, Novinscak T, et al. Effective therapy of transected quadriceps muscle in rat: gastric pentadecapeptide BPC 157. J Orthop Res 2006; 24: 1109-1117.
- Tkalcevic VI, Cuzic S, Brajsa K, et al. Enhancement by PL 14736 of granulation and collagen organization in healing wounds and the potential role of egr-1 expression. Eur J Pharmacol 2007; 570: 212-221.
- Balenovic D, Bencic ML, Udovicic M, et al. Inhibition of methyldigoxin-induced arrhythmias by pentadecapeptide BPC 157: a relation with NO-system. Regul Pept 2009; 156: 83-89.
- Skorjanec S, Dolovski Z, Kocman I, et al. Therapy for unhealed gastrocutaneous fistulas in rats as a model for analogous healing of persistent skin wounds and persistent gastric ulcers: stable gastric pentadecapeptide BPC 157, atropine, ranitidine, and omeprazole. Dig Dis Sci 2009; 54: 46-56.
- Sever M, Klicek R, Radic B, et al. Gastric pentadecapeptide BPC 157 and short bowel syndrome in rats. Dig Dis Sci 2009; 54: 2070-2083.
- Klicek R, Sever M, Radic B, et al. Pentadecapeptide BPC 157, in clinical trials as a therapy for inflammatory bowel disease (PL14736), is effective in the healing of colocutaneous fistulas in rats: role of the nitric oxide-system. J Pharmacol Sci 2008; 108: 7-17.
- Gjurasin M, Miklic P, Zupancic B, et al. Peptide therapy with pentadecapeptide BPC 157 in traumatic nerve injury. Regul Pept 2009; 160: 33-41.
- Vuksic T, Zoricic I, Brcic L, et al. Stable gastric pentadecapeptide BPC 157 in trials for inflammatory bowel disease (PL-10, PLD-116, PL14736, Pliva, Croatia) heals ileoileal anastomosis in the rat. Surg Today 2007; 37: 768-777.
- Sen M, Anadol AZ, Oguz M. Effect of hypercholesterolemia on experimental colonic anastomotic wound healing in rats. World J Gastroenterol 2006; 12: 1225-1228.
- Sikiric P, Seiwerth S, Brcic L, et al. Stable gastric pentadecapeptide BPC 157 in trials for inflammatory bowel disease (PL-10, PLD-116, PL 14736, Pliva, Croatia). Full and distended stomach, and vascular response. Inflammopharmacology 2006; 14: 214-221.
- Pawlik WW, Sikiric P, Brzozowski T, et al. Acceleration of ulcer healing by pentadecapeptide BPC 157 in rats. Involvement of endogenous prostaglandins and gastric secretion. Gastroenterology 2004; 126: 541.
- Jin L, Caldwell RB, Li-Masters T, Caldwell RW. Homocysteine induces endothelial dysfunction via inhibition of arginine transport. J Physiol Pharmacol 2007; 58: 191-206.
- Mozsik G, Sikiric P, Seiwerth S. Pentadecapeptide BPC 157 (PLD116, PL14736, Pliva) influences ATP energy system and antagonizes 0.6 M HCl- and 96% ethanol-gastric lesion in rat. Digestion 2005; 73(Suppl. 2): 41.
- Veljaca M, Lesch CA, Pllana R, Sanchez B, Chan K, Guglietta A. BPC-15 reduces trinitrobenzene sulfonic acid-induced colonic damage in rats. J Pharmacol Exp Ther 1995; 272: 417-422.
- Krivic A, Majerovic M, Jelic I, Seiwerth S, Sikiric P. Modulation of early functional recovery of Achilles tendon to bone unit after transection by BPC 157 and methylprednisolone. Inflamm Res 2008; 57: 205-210.
- Shin IS, Kim JM, Kim KL, et al. Early growth response factor-1 is associated with intraluminal thrombus formation in human abdominal aortic aneurysm. J Am Coll Cardiol 2009; 53: 792-799.