Etiopathogenesis of chronic periodontitis
continues to be unclear. A significant involvement of oral cavity anaerobic
bacteria in aetiology of periodontitis is recognised, in particular involvement
of
Porphyromonas gingivalis,
Tannerella forsythiensis and
Treponema
denticola (1). However, the periodontopathogens may also represent a physiological
component of oral microflora in healthy individuals (2). In turn, the data are
presented indicating that proinflammatory cytokine response of Th17 cells may
play a significant role in pathogenesis of periodontitis, expressed by high
levels of IL-17 and TNF-

in gingival tissue from periodontitis patients (3-5). Nevertheless, till today
it has not been established whether augmented secretion of IL-17 and TNF-

is linked to a specific clinical form of chronic periodontitis. In addition,
recently it has been demonstrated that
Lactobacillus spp. capable of
H
2O
2 production,
may be of importance in prevention against progress of chronic periodontitis
(6, 7). The data indicate that, in turn, oral lactobacilli may restrict development
of inflammatory lesions in chronic periodontitis. Considering the above, this
study aimed at evaluation of IL-17 and TNF-

levels and of oral lactobacilli manifestation, taking into account their ability
to produce hydrogen peroxide, in patients with clinically moderate or severe
chronic periodontitis, in the context of their protective effect on course of
the disease.
MATERIALS AND METHODS
The studies were conducted on 28 patients (28-42 years of age, mean 35.7±3.8 years), among whom two groups were distinguished. Group 1 included 14 patients, (28-42 years of age, mean 35.2±3.6 years; 7 women and 7 men; DMFT - decayed, missing and filled teeth 13.62±2.66) with moderate chronic periodontitis, in whom the average duration of the disease amounted to 20.1±2.1 months (range: 18-25 months). Group 2 included 14 patients (32-42 years of age, mean 36.1±3.7 years; 8 women and 6 men; DMFT 13.53±3.18) with severe chronic periodontitis, in whom the average duration of the disease was 28.1±4.1 months (range: 22-35 months). Group 3 (control) consisted of 15 patients (27-39 years of age, mean 33.9±4.1 years; 8 women and 7 men; DMFT 10.47±3.45) with moderate gingivitis, with the average duration of gingivitis of 2.5±1.2 weeks (range: 1-5 weeks). Start of CP development in the patients was determined in anamnesis conducted with the patient, available cards of disease history and clinical studies. Advancement of periodontitis was determined using WHO criteria, including GI (Gingival Index), PL.I (Plaque Index), PPD (Periodontal Pocket Depth) and CAL (Clinical Attachment Level).
Depth of periodontal pockets was determined on three dental surfaces of every tooth present in oral cavity, using the WHO 621 Hu-Friedy periodontal probe (scale of up to 11.5 mm). During examination, the periodontometer was introduced in parallel to long dental axis, shifting peak of the probe in permanent contact with the tooth, down to the periodontal pocket bottom, recording depth of the periodontal pocket at every surface of the examined tooth. The measurements provided grounds for calculation of the mean periodontal pocket depth in individual patients.
Clinical attachment level (CAL) was measured at 6 surfaces of every tooth using the WHO 621 Hu-Friedy periodontal probe (scale of up to 11.5 mm). The CAL value was calculated on the basis of the measurement establishing the distance between enamel/cementum junction and depth of periodontal pocket. In cases when gingival margin overlapped the enamel/cementum junction two measurements were conducted: the depth of periodontal pocket and the distance between gingival margin and the line of enamel/cementum junction. Deduction of the value representing distance between gingival margin and the line of enamel/cementum junction from the value expressing the depth of periodontal pocket yielded the value orienting us in the site of connective tissue attachment. Data obtained in this way provided basis for calculation of mean CAL value in individual patients (8, 9).
Moderate chronic periodontitis was diagnosed when GI>0, CAL: 3-4 mm and two teeth were present with gingival pockets of >4mm in depth. In turn, patients with severe chronic periodontitis manifested the following variables: GI>0, CAL>5mm and 4 teeth with gingival pockets of >4mm in depth. On the other hand, moderate gingivitis was diagnosed when GI=1.1-2.0; CAL<1 (10, 11).
The investigated material involved gingival crevicular fluid, sampled using
a 1 ml syringe with a thin, blunt, endodontic needle from three deepest periodontal
pockets. The studies included patients in whom sampling of GCF was not followed
by start of periodontological treatment. Before the sampling the patients underwent
no hygienization procedures. For at least 3 weeks earlier the patients used
no drugs (including antibiotics) or antibacterial rinses. The obtained gingival
fluid was tested for presence of IL-17, TNF-

and for manifestation of
Lactobacillus genus, producing or not producing
H
2O
2. Estimations
of gingival fluid (at the 1:10 dilution in PBS) IL-17 and TNF-

levels were conducted by ELISA, using Quantikine Human IL-17 and Quantikine
HS Human TNF-

immunoassay
kits (R&D Systems). Assays were carried out according to the manufacturers
recommendations using human recombinant standards. The minimum detectable concentrations
(sensitivity) in TNF-

assays ranged from 0.038 to 0.191 pg/ml. The minimum detectable concentration
of IL-17 was <15 pg/ml. The optical density was measured at 450 or 490 nm, according
to respective recommendation of manufacturer. At every experiment a standard
curve was drawn basing on the obtained values of optical density (OD) for individual
concentrations of the standards (0-32 pg/ml for TNF-

and 0-500 pg/ml for IL-17). The final result of the studied cytokine concentration
involved a product of the readout on the standard curve (0-32 pg/ml for TNF-

and 0-500 pg/ml for IL-17) and the applied dilution (x10).
In turn,
Lactobacillus spp. was cultured on Rogosa agar and the cultured
isolates obtained in anaerobic conditions were identified using API 50 CHL (bioMerieux).
The capacity of hydrogen peroxide production among
Lactobacillus strains
was defined in culture of the obtained isolates in presence of 5% CO
2
at the temperature of 37°C for 48 hours in a differentiating medium, TMB-Plus
agar, prepared according to Rabe and Hillier (12). Development of an altered
colour of the growing colonies (appearance of a blue colour) indicated production
of hydrogen peroxide.
Results obtained in the studies were analyzed using the computer software STATISTICA
8 for Windows. The statistical analysis included non-parametric tests, permitting
calculation of a broad range of various position measurements (mean) and dispersion
(standard de
viation). In the comparative analysis related to GI, PPD,
CAL and Pl.I and cytokine levels in studied groups the non-parametric Kruskal-Wallis
test and Dunns test were applied. Analysis of the correlation between IL-17
levels and manifestation of oral lactobacilli in CP was conducted using a non-parametric
method based on Spearmans rank correlation coefficients. Significance in frequency
of
Lactobacillus spp. presence is the studied groups was analysed using
the exact Fishers test. In every test, hypotheses were verified at the significance
level of p=0.05.
RESULTS
In the study, the stage of periodontitis advancement was defined using WHO criteria. The obtained values of GI, PPD, CAL indices permitted to distinguish three research groups: group 1 including 14 patients with moderate chronic periodontitis and group 2 including 14 patients with severe chronic periodontitis. Group 3 (control group) included 15 persons with gingivitis.
Statistical characteristics of the obtained mean values of GI, PPD, CAL, PL.I
in the three examined patient groups is shown in
Table 1.
| Table 1. Results
of examined indices in patients with moderate chronic periodontitis (group
1), severe chronic periodontitis (group 2) and in control group with gingivitis
(group 3). |
 |
In both groups of patients periodontal pockets were found to contain high concentrations
of examined cytokines. In the group of patients with moderate chronic periodontitis
(group 1) mean values of IL-17 and TNF-

amounted to, respectively, 19.66±6.1 pg/ml and 4.95±0.91 pg/ml. In turn, in
the group of patients with severe chronic periodontitis (group 2) mean values
of IL-17 and TNF-

amounted to, respectively, 34.7±6.65 pg/ml and 6.94±0.78 pg/ml and were significantly
higher than cytokine levels obtained in group 1 (p<0.0001 and p=0.0003, respectively).
In the control group of individuals with gingivitis (group 3) mean values of
IL-17 and TNF-

amounted to, respectively, 0.65±0.58 pg/ml and 0.17±0.14 pg/ml and were significantly
lower than cytokine levels obtained in group 1 and in group 2 (for all the analyses
p<0.0001). The mean variations of concentrations of cytokine IL-17 and TNF-

and statistical comparisons in the periodontitis group and in the control group
are shown in
Table 2. In analysis of lactobacilli manifestation, presence
of H
2O
2-producing
Lactobacillus spp. was demonstrated in 10 patients of group 1 (71.4%)
while in group 2 two patients (14.3%) carried H
2O
2-producing
Lactobacillus spp. while in 3 patients (21.4%) the isolated
Lactobacillus
spp. bacteria did not produce H
2O
2.
In patients of group 2, with severe chronic periodontitis, a significant decrease
was detected in frequency of
Lactobacillus spp. presence, as compared
to the control group (p=0.0078). Manifestation of
Lactobacillus spp.
and their ability to produce H
2O
2
are shown in
Table 3. In the studies a significant (p=0.0256) negative
correlation (Spearman r=-0.4211) was disclosed between IL-17 levels and frequency
of oral lactobacilli manifestation in CP.
Table 2. Cytokine
levels (IL-17 and TNF- )
in gingival crevicular fluid (GCF) of patients with moderate chronic periodontitis
or severe chronic periodontitis were highly significantly different (p<0.0001
or p=0.0003) between each other and as compared to the control group with
gingivitis (p<0.0001). )
in gingival crevicular fluid (GCF) of patients with moderate chronic periodontitis
or severe chronic periodontitis were highly significantly different (p<0.0001
or p=0.0003) between each other and as compared to the control group with
gingivitis (p<0.0001). |
 |
| Table 3. Capacity
to form H2O2
in the obtained Lactobacillus spp. isolates and statistical significance
(p) of differences in frequency of Lactobacillus spp. presence. |
 |
DISCUSSION
Population of Th17 cells is characterized by secretion of mainly IL-17, and
also of other proinflammatory cytokines, including TNF-

,
IL-22 and IL-26 (13). IL-17 induces recruitment of neutrophils together with
inflammatory reaction, which in addition is synergically amplified by TNF-

,
IL-22 and IL-26. Moreover, IL-17 triggers neutrophilia while IL-22 induces anti-microbial
peptides, providing a nonspecific immune response against bacterial and fungal
pathogens (14-17). Thus, the cytokine response of Th17 cells plays an important
role in host defense, and may represent also a principal mediator in pathogenesis
of several inflammatory diseases, as shown by results of recent years (3, 12,
17-19). In our studies, presented in this paper we have demonstrated a marked
increase in levels of IL-17 and TNF-

in gingival crevicular fluid in patients with either moderate or severe chronic
periodontitis, even if in the latter the estimated cytokines level was significantly
higher. Such an elevation of IL-17, as well as of TNF-

levels in chronic periodontitis was earlier described also by other authors
(3-5). Nevertheless, in this study for the first time overproduction of IL-17
and TNF-

have been
shown to be typical for both the defined clinical forms of moderate and severe
chronic periodontitis. In parallel, the obtained results have permitted to distinguish
patients with a high cytokine response of Th17 cells (representing the high
responders) and those with moderate response of Th17 cells (representing moderate
responders). In moderate responders the increase in maximum cytokine levels
has not exceeded the 20-fold maximum values in the control group. In patients
representing the high responders the increase in maximum cytokine levels corresponded
to the same or higher level than that representing 20-fold maximum level in
the control group. Intensity of Th17 cell cytokine response, high or moderate,
corresponded to severe or moderate clinical form of chronic periodontitis. Therefore,
it can be concluded that chronic periodontitis is determined by persisting cytokine
response of Th17 cells, the intensity of which may be significant for further
clinical course of the disease. In part, the conclusion is supported by the
data demonstrating dependence of joint damage progression in rheumatoid arthritis
patients upon high production of IL-17 and TNF-

(20). In studies conducted
in vitro the periodontopathogens were demonstrated
to induce cytokine response of Th17 (21). Therefore, it is possible that Th17
cells play an important physiological indirect role, controlling periodontal
colonization by microbes and periodontopathogens in particular. Probably, the
effect of the function includes low gingival levels of IL-17, detected also
in this study in patients with gingivitis. A marked increase in cytokine response
of Th17 cells seems to result from disturbances in its intracellular control
or strong expression of target genes due to their transcriptional activation
by periodontopathogens. Until now, the intracellular signalling pathway that
regulates IL-17 production remains unknown. Nevertheless, the nuclear factor
kappa B (NF-
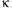
B)
was shown to be involved in overproduction of IL-17 (22). Therefore, the final
result of activated secretory function of Th17 cells may be dependent on expression
of IL-17 gene. Polymorphism of IL-17 gene might determine overproduction of
IL-17, as well as the NF-
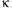
B-dependent
secretion of several proinflammatory, which cooperate with IL-17.
In present studies, manifestation of hydrogen peroxide-producing
Lactobacillus
spp has been demonstrated in most patients of the control group as well
as in patients with moderate chronic periodontitis in gingival crevicular fluid.
On the other hand, in gingival fluid of patients with severe chronic periodontitis
Lactobacillus spp. has been detected in only 5 persons and in only 2
of them this pertained H
2O
2-producing
strains. However, high gingival concentrations of IL-17 and TNF-

have been disclosed in all patients with severe chronic periodontitis. Moreover,
the study has demonstrated negative correlation between levels of IL-17 in GCF
on one hand and manifestation of oral lactobacilli on the other. Therefore,
it can be concluded that a very pronounced cytokine response of Th17 cells,
linked to severe chronic periodontitis, exerting proinflammatory and antibacterial
effect reduces in a secondary way manifestation and metabolic activity of oral
lactobacilli. In turn, the moderate IL-17 cytokine level may be insufficient
for induction of a nonspecific immune response, leading to elimination of H
2O
2-producing
oral lactobacilli, the presence of which has seemed to reduce secretory activity
of Th17 cells as well to restrict growth of periodontopathogens and, therefore,
to prevent against progression of chronic periodontitis. The suggestion seems
to be verified by experimental studies, which show that
Lactobacillus
strains may exert immunomodulatory effect, acting in a suppressive way on expression
of genes coding for proinflammatory cytokines or in a regulatory manner on human
dendritic cells (23-25). Moreover, activity of anti-inflammatory probiotic strains
of
Lactobacillus was noted on urogenital tract mucosa and activity of
E. coli Nissle on gastric mucosa were detected (26,27). Recently, strongly
antagonistic interaction of oral lactobacilli to Gram-negative periodontal pathogens,
Porphyromonas gingivalis and
Aggregatibacter actinomycetemcomitans
(28) was documented.
Results presented in this study indicate that development of chronic periodontitis
are linked to persisting cytokine response of Th17 cells, the intensity of which
may shape clinical course of the disease. In parallel, H
2O
2-producing
oral lactobacilli may prevent against progress of chronic periodontitis, most
probably restricting secretory activity of Th17 cells and growth of periodontopathogens.
The data provide rationale for further studies aimed at implementing a new strategy
in therapy of chronic periodontitis, considering the role of lactic acid bacteria
in severe forms of the disease.
Acknowledgements:
This study was supported by the University of Medical Sciences in Poznan, Poland
(Grant no. 502-01-02206316-0002658 and, partially, Grant no. 501-01-2209324-07058).
Conflict of interest: None declared.
REFERENCES
- Holt SC, Ebersole JL. Porphyromonas gingivalis, Treponema denticola, and Tannerella forsythia: the red complex, a prototype polybacterial pathogenic consortium in periodontitis. Periodontology 2000 2005; 38: 72-122.
- Ledder RG, Gilbert P, Huws SA, et al. Molecular analysis of the subgingival microbiota in health and disease. Appl Environ Microbiol 2007; 73: 516-523.
- Vernal R, Dutzan N, Chaparro A, Puente J, Valenzuela MA, Gamonal J. Levels of interleukin-17 in gingival crevicular fluid and in supernatants of cellular cultures of gingival tissue from patients with chronic periodontitis. J Clin Periodontol 2005; 32: 383-389.
- Cardoso CR, Garlet GP, Crippa GE, et al. Evidence of the presence of T helper type 17 cells in chronic lesions of human periodontal disease. Oral Microbiol Immunol 2009; 24: 1-6.
- Santos VR, Ribeiro FV, Lima JA, Napimoga MH, Bastos MF, Duarte PM. Cytokine levels in sites of chronic periodontitis of poorly controlled and well-controlled type 2 diabetic subjects. J Clin Periodontol 2010; 37: 1049-1058.
- Szkaradkiewicz AK, Tukiendorf B, Stopa J. Oral lactobacilli and periodontitis. Clin Microbiol Infect 2006; 12: 0371.
- Szkaradkiewicz AK, Stopa J. Lactobacillus spp. of oral cavity microflora in chronic periodontitis. Pol J Environ Stud 2008; 17: 236-242.
- Listgarten MA, Mao R, Robertson P. Periodontal probing and the relationship of the probe tip to periodontal tissues. J Periodontol 1976; 47: 511-513.
- Benamghar L, Penaud J, Kaminsky P, Abt F, Martin J. Comparison of gingival index and sulcus bleeding index as indicators of periodontal status. Bull World Health Organ 1982; 60(1): 147-151.
- Koll-Klais P, Mandar R, Leibur E, Marcotte H, Hammarstrom L, Mikelsaar M. Oral lactobacilli in chronic periodontitis and periodontal health: species composition and antimicrobial activity. Oral Microbiol Immunol 2005; 20: 354-361.
- http://www.whocollab.od.mah.se
[accessed on 25 November 2009] WHO Oral Health Country/Area Profile Programme.
WHO Headquarters Geneva and WHO Collaborating Centre - Malmo University,
Sweden.
- Rabe LK, Hillier SL. Optimization of media for detection of hydrogen peroxide production by Lactobacillus species. J Clin Microbiol 2003; 41: 3260-3264.
- Khader SA, Gaffen SL, Kolls JK. Th17 cells at the crossroads of innate and adaptive immunity against infectious diseases at the mucosa. Mucosal Immunol 2009; 2: 403-411.
- Zenewicz LA, Flavell RA. IL-22 and inflammation: Leukin through a glass onion. Eur J Immunol 2008; 38: 3265-3268.
- Wilson RH, Whitehead GS, Nakano H, Free ME, Kolls JK, Cook DN. Allergic sensitization through the airway primes Th17-dependent neutrophilia and airway hyperresponsiveness. Am J Respir Crit Care Med 2009; 180: 720-730.
- Conti HR, Shen F, Nayyar N, et al. Th17 cells and IL-17 receptor signaling are essential for mucosal host defense against oral candidiasis. J Exp Med 2009; 206: 299-311.
- Cho JS, Pietras EM, Garcia NC, et al. IL-17 is essential for host defense against cutaneous Staphylococcus aureus infection in mice. J Clin Invest 2010; 120: 1762-1773.
- Sato K, Suematsu A, Okamoto K, et al. Th17 functions as an osteoclastogenic helper T cell subset that links T cell activation and bone destruction. J Exp Med 2006; 27: 26732682.
- Duarte PM, da Rocha M, Sampaio E, et al. Serum levels of cytokines in subjects with generalized chronic and aggressive periodontitis before and after non-surgical periodontal therapy: a pilot study. J Periodontol 2010; 81: 1056-1063.
- Kirkham BW, Lassere MN, Edmonds JP, et al. Synovial membrane cytokine expression is predictive of joint damage progression in rheumatoid arthritis: a two-year prospective study (the DAMAGE study cohort). Arthritis Rheum 2006; 54: 1122-1131.
- Oda T, Yoshie H, Yamazaki K. Porphyromonas gingivalis antigen preferentially stimulates T cells to express IL-17 but not receptor activator of NF-kappaB ligand in vitro. Oral Microbiol Immunol 2003; 18: 30-36.
- Kim KW, Cho ML, Park MK, et al. Increased interleukin-17 production via a phosphoinositide 3-kinase/Akt and nuclear factor kappaB-dependent pathway in patients with rheumatoid arthritis. Arthritis Res Ther 2005; 7: R139-R148.
- Inoue R, Otsuka M, Nishio A, Ushida K. Primary administration of Lactobacillus johnsonii NCC533 in weaning period suppresses the elevation of proinflammatory cytokines and CD86 gene expressions in skin lesions in NC/Nga mice. FEMS Immunol Med Microbiol 2007; 50: 67-76.
- Vissers YM, Snel J, Zuurendonk PF, Kleerebezem M, Wichers HJ, Savelkoul HF. Lactobacillus strains differentially modulate cytokine production by Lactobacillus hPBMC from pollen-allergic patients. FEMS Immunol Med Microbiol 2011; 61: 28-40.
- Gad M, Ravn P, Soborg DA, Lund-Jensen K, Ouwehand AC, Jensen SS. Regulation of the IL-10/IL-12 axis in human dendritic cells with probiotic bacteria. FEMS Immunol Med Microbiol 2011; 63: 93-107.
- Konturek PC, Sliwowski Z, Koziel J, et al. Probiotic bacteria Escherichia coli strain Nissle 1917 attenuates acute gastric lesions induced by stress. J Physiol Pharmacol 2009; 60(Suppl 6): 41-48.
- Cadieux PA, Burton JP, Devillard E, Reid G. Lactobacillus by-products inhibit the growth and virulence of uropathogenic Escherichia coli. J Physiol Pharmacol 2009; 60(Suppl 6): 13-18.
- Teanpaisan R, Piwat S, Dahlen G. Inhibitory effect of oral Lactobacillus against oral pathogens. Lett Appl Microbiol 2011; 53: 452-459.


